Delivering affordable, universal access to healthcare for the 5.8 billion people currently living in emerging countries is one of the key challenges facing the world today. In addition to this, according to the World Health Organisation (WHO), three out of four chronic diseases are most prevalent in these low or middle income countries.
Creating the necessary infrastructure to deliver patient-centred, value care is a task acknowledged to be beyond many governments to handle alone; however, the 2020 Zayed Sustainability Prize Health Category finalists are proving that small to medium-sized businesses and non-profit organisations can support such efforts. The solutions and innovation being invested by these organisations is also addressing many of the 17 UN Sustainable Development Goals (SDGs). With regards to affordable healthcare, the core goals are SDG1, SDG 2, SDG 6, and SDG17.
In the Q&A that follows, the 2020 Health Category finalists, along with Jeremy Laurance, Selection Committee Member for the Prize’s Health Category, provide their take on the key issues relating to the challenges and meeting the United Nations’ SDG 2030 targets.
1) According to Deloitte’s 2019 Global Health Care Outlook report, new patient care delivery models have helped improve access to and affordability of healthcare – and this way forward offers the greatest potential to positively impact health outcomes in the future. Do you agree?
If yes, please elaborate on how your organisation’s solution demonstrates this point. If not, is there another approach that you think will enable underprivileged communities to become healthier in the long-run?
Helena Samsioe, CEO of GLOBHE:
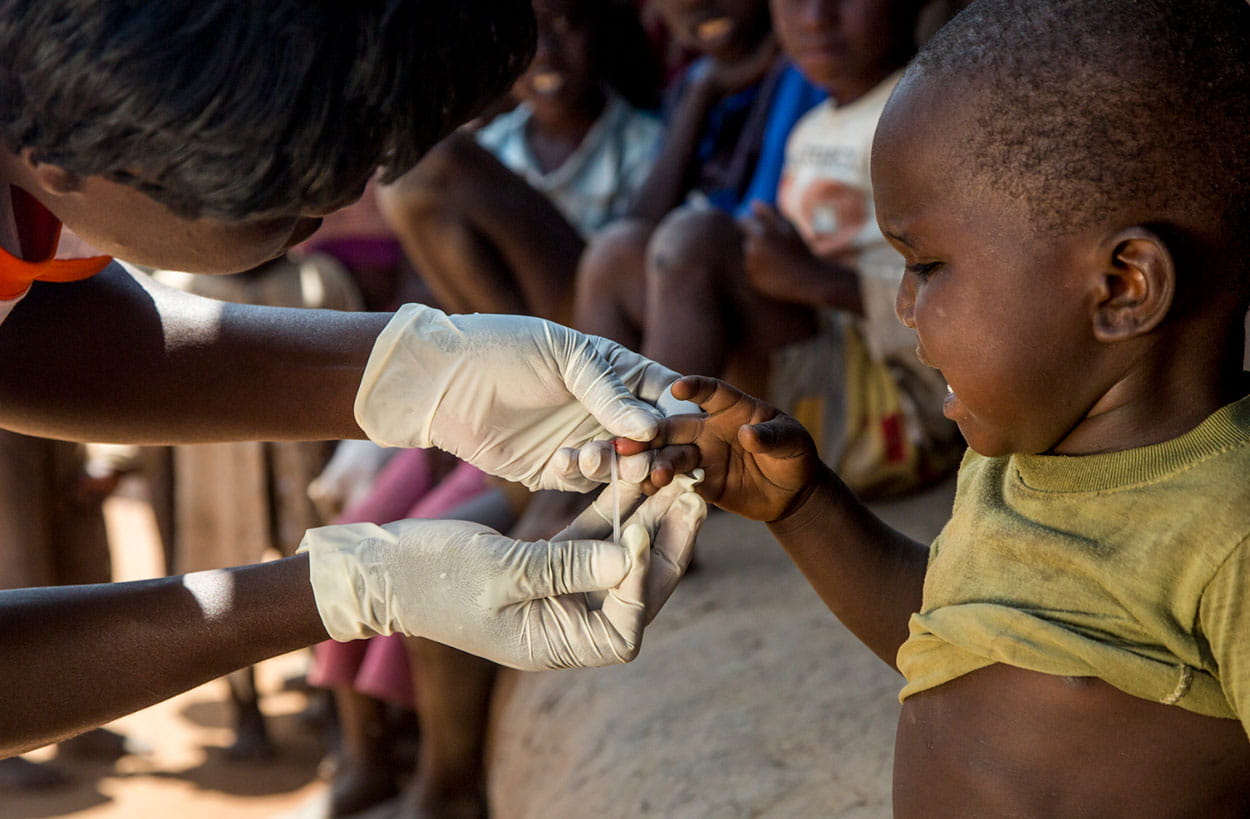
It is part of the solution, but many times we still forget to start from the beginning, meaning that we forget basic but crucial fundamentals such as updated population data. If we take a decision based on old or incomplete data, then all the actions that follows will be more or less faulty. We got to experience this first hand during a cholera outbreak, in Malawi last year, where the number of people living in the affected area was unknown due to old data, so it was difficult to know how much Cholera vaccine was needed.
Our solution was then used to provide an updated drone map that consisted of over 50,000 drone images over the area where households were automatically marked and counted by using AI, providing UNICEF and the Malawi Ministry of Health with updated population data so the response could be planned for more efficiently.
Lila Cruikshank, Director of Business Development at One Family Health:
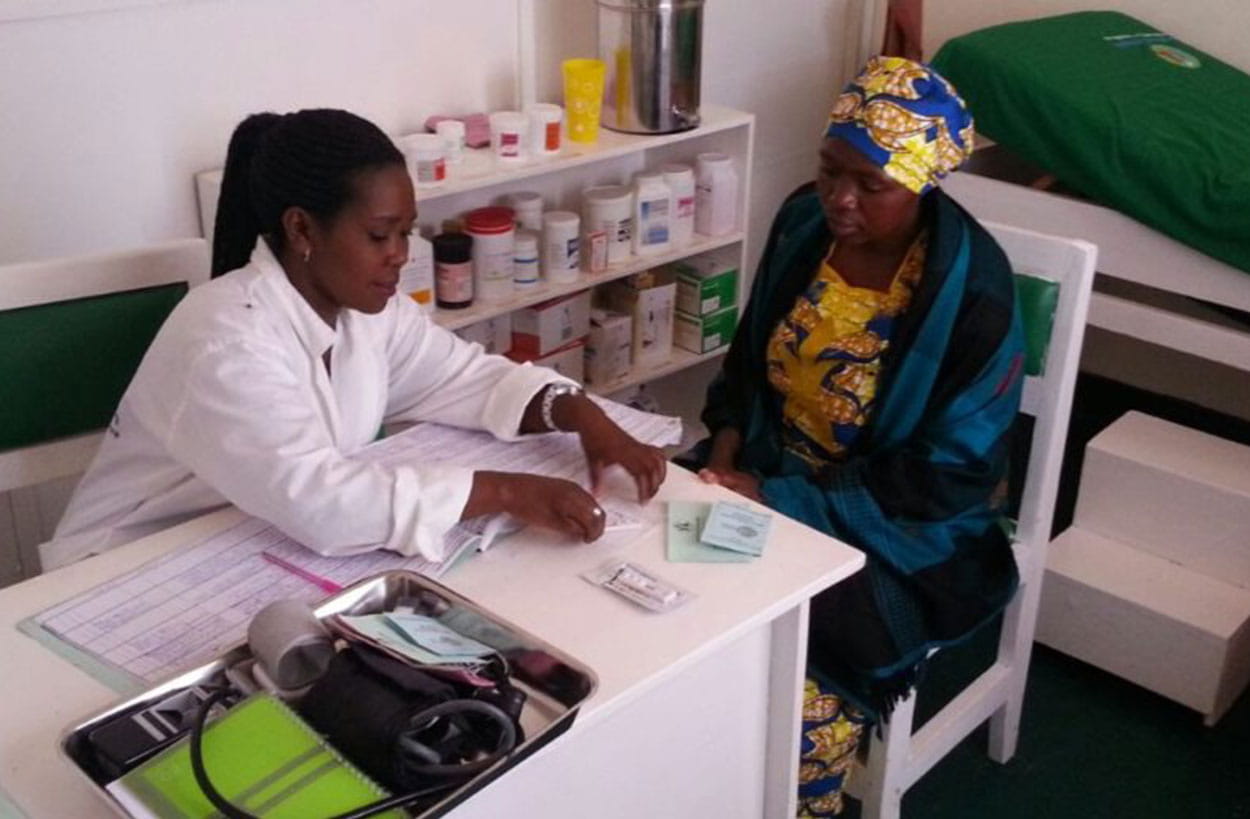
Innovation in healthcare delivery and business models is critical in order to overcome barriers of geography, socioeconomics, and limited public sector resources to increase the accessibility, affordability, and quality of healthcare. OFH’s model is one such innovation – bringing together a franchise approach with a public-private partnership strategy, undergirded by a powerful digital platform. By harnessing the entrepreneurial potential of nurse-franchisees, OFH creates incentives for nurses to live and work in rural areas underserved by existing health facilities, reducing critical geographic barriers to accessing healthcare and essential, life-saving medicines.
Alain Nteff, Co-founder and Director of GiftedMom:
I agree with Deloitte’s 2019 Global Health Care Outlook report that new patient care delivery models have helped improved access to and affordability of healthcare. One channel playing a huge role to democratise access to healthcare are mobile phones, owned by 80% of Africans. At GiftedMom, we’ve been able to deploy a life-saving health education service, provide pregnant women and new mothers unlimited access to a doctor using SMS, USSD and voice messages which can reach even moms at the last mile. This has drastically increased the number of pregnant women who complete at-least 4 antenatal care before delivery and number of babies completely vaccinated. Furthermore, smartphone penetration is growing +30% yearly, meaning in the coming years, we’ll be able to diagnose disease, consult and prescribe drugs via phone. This reduces investment in brick-and-mortar and will drive down the cost of accessing care.
2. The 2019 UN General Assembly reached a comprehensive agreement on global health for the first time in history— with a goal to achieve Universal Health Coverage for all by 2030. This means that all people regardless of their ability to pay, should have access to the healthcare they need, when and where they need it, without facing financial hardship.
In your opinion, how can we ensure that we are going to meet this expectation of universal healthcare coverage?
Helena Samsioe, CEO of GLOBHE:
Access to quality data is going to be key. If we do not have population data – we will not know if they are reached by healthcare or not. A few years ago, there was news about Malaria being on the rise in Rwanda, even though effective methods to combat malaria had been made. It turned out that Malaria was most likely not on the rise but instead there was now more efficient data tracking methods so that people who got malaria were now registered at a higher rate. Besides quality data, prevention is key. It will most likely be impossible to reach Universal Health Coverage for all unless even more focus is turned towards prevention. Our solution is being used to early identify malaria mosquito breeding sites by drones making it possible to more accurately spray where it is needed, and more efficiently plan a malaria prophylax roll out.
Lila Cruikshank, Director of Business Development at One Family Health:
Innovation in service delivery models and in financing healthcare will be critical to reduce the costs of healthcare delivery in order to achieve the critical and ambitious goals of achieving Universal Health Coverage. The Government of Rwanda is a pioneer in creating a national health insurance scheme with tiered premiums that make healthcare accessible to the poorest Rwandans. OFH’s model, which has partnership with the Government of Rwanda as its foundation, leverages private sector principles and mobilizes private capital to reduce the cost of delivering quality care, enabling OFH and the Government of Rwanda to increase access to affordable healthcare at a lower cost.
Alain Nteff, Co-founder and Director of GiftedMom:
Universal Health coverage (UHC) can be achieved in the next 10 years. A key driver will be adoption of new technologies like blockchain, which provides a quick and transparent way of moving cash from point A to B. Today, some African governments like Cameroon have a new outcomes-based program where health structures are given bonuses if they deliver quality care. The challenge is the long payment cycle (cash leaving government coffers to these structures), an issue which has greatly handicapped this initiative. If we rely on manual logistics to reimburse health structures for free healthcare given to the population, the long payment cycles and potential “leakages” as the cash moves, will handicap the quality of care and jeopardise our vision of UHC. GiftedMom is experimenting with blockchain technology to finance antenatal care consultations and medical exams of pregnant women who can’t afford care in rural areas. At scale, this can greatly contribute to making UHC possible.
3) Today’s healthcare consumers are expecting solutions that are more coordinated, convenient, customised, and accessible. In your opinion, has the entry of disruptive technologies, revamped payment models and non-traditional competitors, impacted consumer healthcare and access to healthcare for the better? If not, what is still lacking? Please elaborate on your opinion.
Jeremy Laurance, former Health Editor at The Independent, Selection Committee Member (Health Category):
Most innovations in health follow a similar trajectory. There is a honeymoon period when people say it is transformative and usage rises. Then problems emerge and usage plummets. Finally, people acknowledge that it is a step forward but has some drawbacks - and usage stabilises.
The impact of technological innovation on health has been a story of two steps forward, one step back. We must be positive enough to embrace new ways of doing things when they are introduced, while remaining sceptical enough to spot problems when they arise. For example, an app that allows you to consult a doctor remotely via your mobile phone represents a big improvement in convenience and accessibility. But is there a cost in terms of the quality of the consultation and examination? If the answer is yes - and this seems likely - then we must ask if the gain in convenience outweighs the loss in quality. Technology advances but the questions remain the same.
.svg?iar=0&hash=670E3638BC16C0DD69B262DD1184DEA8)